REVERSE SHOULDER REPLACEMENT
- Home
- REVERSE SHOULDER REPLACEMENT
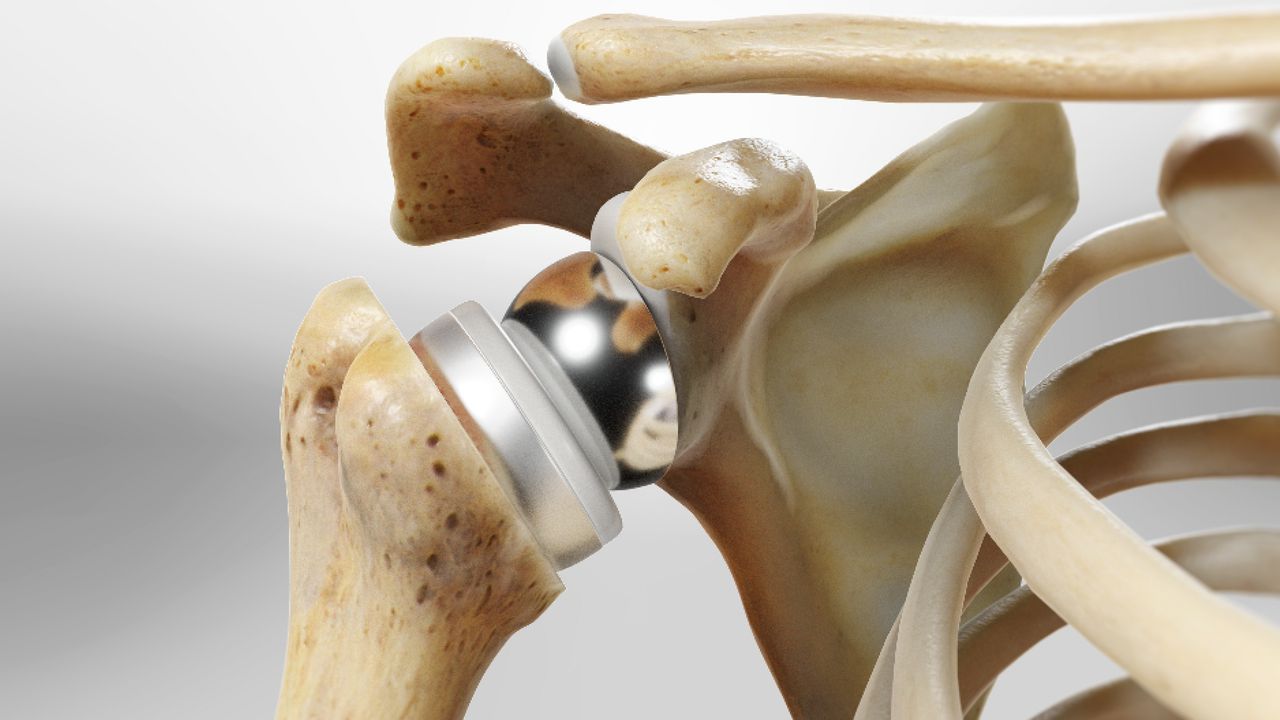
What is Reverse Shoulder Replacement Surgery:
In a reverse shoulder replacement surgery, the holder and metal balls are interchanged. The metal ball is fixed to the holder and the plastic cup is implanted to the top end of the humerus.The reverse shoulder replacement surgery having better outcomes for sufferer with the cuff tear joint disease because it lies on various muscles to push the arms. In addition, For a good and healthy & strong shoulder, the rotator cuff muscles improve position and influence the arm through the range of movement. A conventional replacement surgery also utilizes the rotator cuff muscles to perform action properly. Therefore, A sufferer with a larger cuff tear arthropathy and rotator cuff tear, these muscles perform no large function. As a result, reverse shoulder replacement lies on the deltoid muscles, rather than of the rotator cuff, to influence and locate the arm.
Symptoms & Causes:
Following are the symptoms or cause where a doctor prescribed Reverse shoulder replacement surgery.
Cuff tear arthropathy.
While Totally split the rotator cuff, can’t be fixed or operated.
Due to the unsuccessful past shoulder replacement surgery.
Having shoulder discomfort or pain and trouble to uplifting the arm off regarding your side or above your head.
Due to a complicated break in the shoulder joint.
Feeling a constant shoulder pain or dislocation.
Have swelling in the shoulder joint.
Attempted other methods or approaches, like take the rest, pills, cortisone vaccinations, and natural therapy, that haven’t reduced or helped in shoulder pain.
When a sufferer’s rotator cuff tear cannot improve and many changes in shoulder mobility. Your affected shoulder may feel deadened or paralyzed.
Stiffness in the affected shoulder.
Recovery after reverse shoulder replacement surgery:
After completed reverse shoulder replacement surgery, your pharmaceutical team will give you various doses of antitoxins to decrease your hazard of infection, and painkillers to hold you relaxed. Most sufferers are capable to eat heavy food and stand out of bed the day after complete surgery. The sufferer will most be ready to go home on the 2-3 days after surgery.
Improvement at home:
When you are ready to go to the hospital and home, your operated shoulder will be in a dressing. Your consultant may give some instruction to you to do the soft scale of movement activities to improve your versatility and toughness. To increase the adaptability and elasticity, A regular physical treatment may also be prescribed by the doctor.The sufferer may be ready to comb, feed, and dress inside some weeks after successful surgery.
Do’s and Don’ts After Surgery:
Doing regularly home exercise schedule suggested by your physician.
Don’t pull out and push heavy things than 2 kilograms, for the starting 6 weeks after completed surgery.
Don’t play in heavy lifting after reverse shoulder replacement surgery.
To ignore difficult arms situations, such as back your body and arm vertical out to the side to the starting first 5-6 weeks.
Do the exercise 2-3 times in a day as prescribed by the doctor.
Don’t use your operated shoulder to push out yourself up from a bed or chair. Because this needs powerful muscle reductions.
Long-term results or outcomes:
After improvement and recovery, you will be ready to raise your operated shoulder to just up shoulder height and twist the elbow to touch the top of your head. Reverse shoulder replacement surgery gives excellent effort in relief due to the pain and sufferer satisfaction is very high.
In addition, If you are looking for a reverse shoulder replacement surgery doctor, Please contact Dr. Harish Talreja, the best reverse shoulder replacement doctor in Jaipur.
Call Us Today for Consultations
Feel free to pay us a visit. You won’t regret it for sure.










