CAUSES, SYMPTOMS AND TREATMENT KNEE SYNOVITIS
- Home
- CAUSES, SYMPTOMS AND TREATMENT KNEE SYNOVITIS
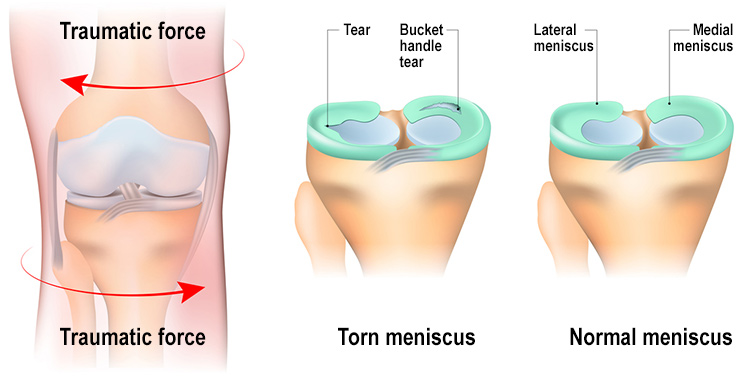
Knee Synovitis Treatment in Jaipur
Knee Synovitis is a constant knee pain condition that involves swelling in the knee. Our knees are girded by soft tissues. When this soft tissue becomes infected, this infection is known as synovitis. The knee joint is filled with a layer known as synovial membrane, which oils the knee joint to work smoothly. When the synovial membrane is infected or inflamed, the synovial membrane does not work properly and knee joint becomes damaged.
Causes of Knee Synovitis
In synovitis, synovial membrane, which lines and greases the knee joint, becomes infected. Synovitis of the knee can be an effect on other body joints and increase the chances to will have rheumatoid arthritis. Almost Synovitis happens due to infection in the synovial membrane. Infection in the knee is due to physical internal joint bleeding. Continues bleeds create a thickening of blood veins nearby the damaged joint. That is why the knee joint will start to swell by infection.
Symptoms and signs of Knee Synovitis
Any type of pain, redness, and swelling in the knee is a starting symptom of synovitis. After any damage, your knee may start to swell. The joint has infected due to bleeding and this bleeding causes hurt, damaged tissues and swelling on the knee.
Commonly having pain in the knee.
Having swelling in the knee.
Feel hardness and stiffness in the knee.
Redness and color change(Pink) in an affected area.
Feeling warmness and hotness in the knee.
Continues knee pain.
Also, Having pain and difficulty moving the knee.
How to prevent knee synovitis?
The best way to avoid or prevent the knee synovitis symptoms is to defend your knees from damage. In case of an damage or internal bleeding, take care of your knee before the pain and condition turn permanent problem.
Do knee Stretching exercise daily
Especially, Prevent serious damage
Avoid sudden force or stress on knee joint
take care if internal bleeding happens
Treatment for knee synovitis
The knee synovitis treatment method depends on the basis of the synovitis. RICE technique (Rest, ice, compression, and elevation) apply in case of the hit from the heavy things.
If the synovitis becomes an arthritis problem, then anti-infected medicines are normally thriving. If the knee synovitis becomes more serious problems and the above points are not effectively work on pain, reduce the pain, then firstly concern with the knee specialist doctor. An arthroscopic operation may implement to eliminate the injured synovial tissue or the pinching portion of the lining. As a result, If you are having knee synovitis please contact Dr. Harish Talreja – the best Knee arthroscopy doctor in Jaipur
Call Us Today for Consultations
Feel free to pay us a visit. You won’t regret it for sure.










